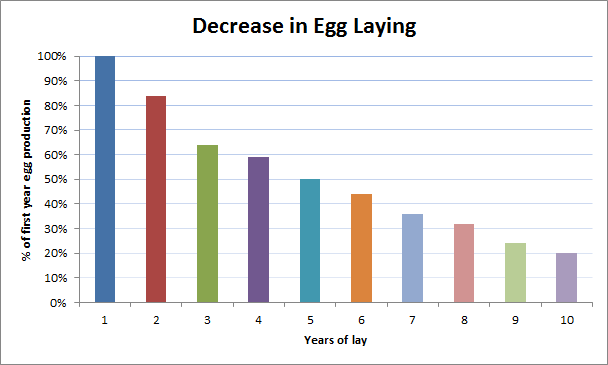Last week I spoke with a woman who I think is in her early 40s who is starting rapamycin to maintain her fertility (slow, or prevent ovarian aging) and prevent / delay menopause. She will be writing about the process, and the results over the coming months and I’ll provide a link to her articles when they come out.
But this got me thinking and I’m wondering if there are other women here who might be taking rapamycin to either enhance their fertility (maintain their fertility as they age past 30) or for menopause prevention. Please post your experience if you are.
Following is some research on how rapamycin has proven to help in fertility:
Fertility
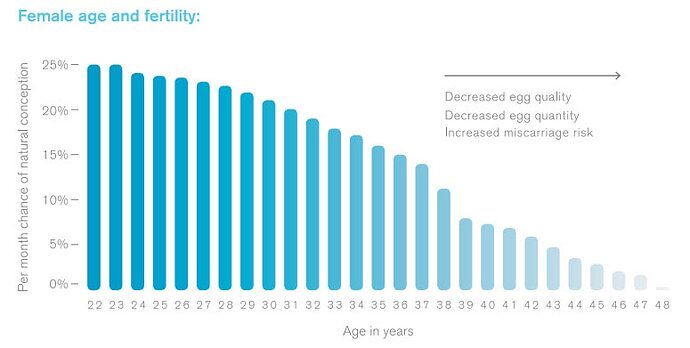
In terms of female fertility, there is already strong evidence in mice and rats that rapamycin delays (reverses?) reproductive aging in females.
Note: Matt Kaeberlein touches upon rapamycin / mtor pathway and ovarian aging in this new presentation on the current state of the science around Rapamycin. An interesting comment Matt makes related to ovarian aging was he was at a recent conference on reproductive aging and there were 3 or 4 presentations on how mTOR was involved in ovarian aging. He notes that he saw a presentation where:
“they had remarkable pictures with old mice and atrophied ovaries, and then you look at an old mouse that had been treated with rapamycin and the ovaries look like young ovaries from a young mouse.”
I’ve positioned the video to the exact spot where reversing ovarian aging / function is discussed, below: Targeting aging with rapamycin: On the path toward 21st Century Medicine - YouTube
Here are some research studies that report this benefit:
- Short‐term rapamycin treatment increases ovarian lifespan in young and middle‐aged.
- Rapamycin can preserve the developmental potential of eggs.
- Rapamycin can maintain the developmental potential of eggs (full paper, PDF)
- Rapamycin keeps the reproductive clock ticking.
- Rapamycin prolongs female reproductive lifespan.
- Effect of caloric restriction and rapamycin on ovarian aging in mice
The inhibition of mTOR signaling can also prolong ovarian lifespan. Compared to that in control rats, rapamycin-treated rats have a 2-fold increase in the number of primordial follicles after 10 weeks of treatment with rapamycin (5 mg/kg every other day, i.p.) (17, 111). These results indicate that rapamycin can protect the ovarian reserve and extend ovarian lifespan. An interesting experiment also showed that a transient 2-weeks regimen of rapamycin facilitates the sufficient extension of ovarian lifespan in mice regardless of the age at treatment initiation.
[Note: other compounds like Ca-AKG and NMN seem to also help with preservation of fertility (sources: 1, and 2). So perhaps an ideal approach would be to combine these three approaches.]
There are researchers who argue that rapamycin effectively “slows down time” from a biological growth and development perspective - while maintaining that potential for growth in the future. I’ve spoken to some academics at major US universities that are planning more studies focused on rapamycin and human fertility so its an area ripe for more research, but the preliminary evidence is very encouraging. It seems to me that preservation of fertility is easier and more likely than reversal of fertility loss, but of course, I could be wrong.
Menopause
If rapamycin is slowing fertility declines, then it suggests that it might also delay or prevent menopause. Delayed menopause has many benefits and is associated with a longer life overall for women.

Source: The time is now: Regular exercise maintains vascular health in aging women
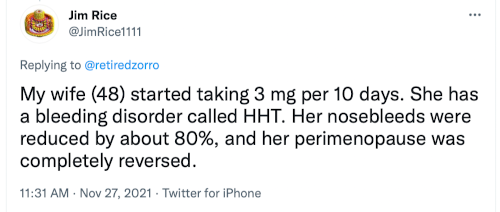
And while there is no research on this published that I can find, there are anecdotal reports that people are seeing positive results and delay of menopause with rapamycin:
I have been taking rapamycin for 6 months on and off. It has improved my hdl and ldl ratio to the point where my hdl is now higher than my ldl. I have also been giving it to my mother who is 63 years of age. She rather unwillingly told me that she has been having her period again for the first time in 14 years. Now that is a turn up for the books and can hardly be seen as placebo or coincidence
I just wanted to inform the group of an interesting ongoing small pilot study I’ve been doing at home. I’ve been feeding my chickens that I purchased in 2017 as chicks, rapamycin for the past two years on a periodic (weekly) basis. One of the chickens died last year due to a plugged duct, which is a common problem. But prior to that, and with the one remaining chicken that is now on year 4 of egg production, the daily egg product is still up at the 90% to 95% daily laying schedule that is typical only of much younger chickens - 1 year olds, for example (see below). So my 4 year old chicken is laying eggs like a 1 year old chicken. Obviously, N=1 doesn’t mean too much, but the indication seems quite positive and supports all the research mentioned above.
What the Typical Egg Laying Ability Trend Line is for Chickens (No Rapamycin)