A few lab results…
Rapamycin after 48 hours
After my issue with the compounding pharmacy (see Biohacking rapamycin’s bioavailability), my MD wrote me a new script for a generic Sirolimus. I posted a photo on the linked thread.
I’ve started at 14 mg once per week, 2 mg over what I took prior to the compounding pharmacy mess.
I should have everything on track, but the experience piqued my skepticism, so I had a test done.
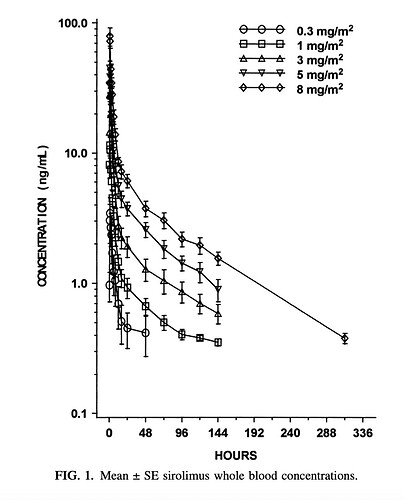
Because of access to the blood draw and scheduling I had blood taken 48 hours after my weekly dosing (of 14 mg). Not looking for maximum or minimum levels. I just want to make certain I get reasonable levels.
Results → Sirolimus, Lc/ms/ms (mcg/L) = 4.6
Does this give me the blood levels I should expect taking US sourced generic Sirolimus 48 hours after dosing?
Probably a month or more before the rapamycin kicks in again, but I had the following tested as well:
hs CRP: 0.6 mg/L
Apolipoprotein A1: 146 mg/dL
Apolipoprotein B: 146 mg/dL
This give me a ratio of 1.00 which seems concerning.
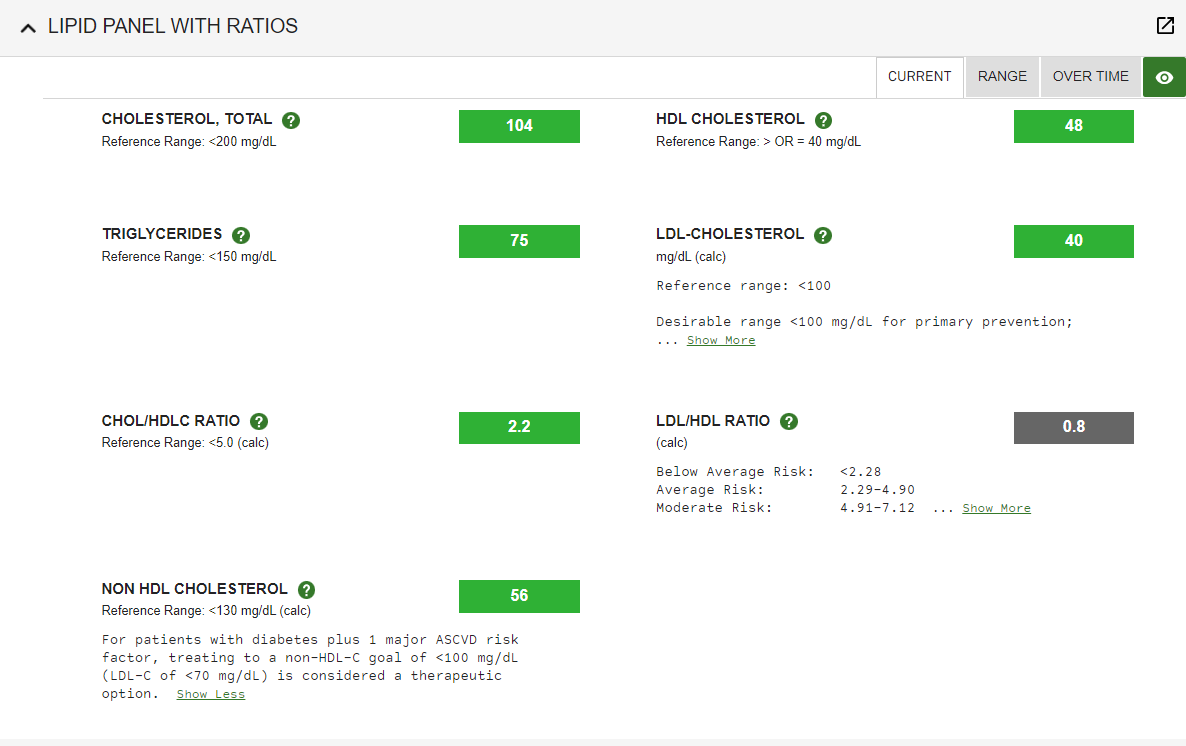
Cholesterol
- Total: 282
- HDL: 58
- LDL: 201
- VLDL: 22
Yet, I have no coronary calcium and a clear carotid artery.
I’d appreciate some interpretation of the results and suggestions.
Thanks in advance.