Using DEP instead of injection for calcium hydroxiappatite moots the risk of vascular occlusion. That product — radiesse — has been amazing for me. Also hifu and rf microneedling — those are theoretical concerns but in practice only valid if the practitioner is a complete ding dong who doesn’t understand facial anatomy. You need to match the right depth to the right area and be conservative with the energy settings. Thinner faces even more so. I have a high cheek boned wide face with some fullness. A bit of fat loss in the face is DESIRABLE for me and I’ve used both rf microneedling and hifu for years with nothing but great results. My face looks younger now than in 2022 when I started. Those devices won’t melt your face or anything unless you do something really stupid. And you’d feel pain and stop. Maybe some people get numbed and can’t give live feedback of terrible pain. There’s zero need for numbing with these modalities.
Erasing Years Of Skin Damage Anywhere In Minutes!
I. Executive Summary
The provided transcript features a cosmetic influencer detailing an over-the-counter (OTC) topical regimen for photoaging, dyschromia, and hyperpigmentation. The core thesis is that a combination of kojic acid, tranexamic acid (TXA), and niacinamide can reverse ultraviolet (UV)-induced melanin accumulation. While the biological plausibility of the active ingredients is well-documented in dermatological literature, the speaker’s clinical claims are heavily compromised by cosmetic hyperbole and physiological inaccuracies.
Specifically, the assertion that tyrosinase inhibitors like kojic acid yield visible depigmentation upon the “very first” application is biologically impossible; epidermal turnover requires approximately 28 to 40 days for visually perceptible reduction in melanin deposition. However, the foundational claim that UV radiation drives 80% of visible skin aging (photoaging) is accurate and supported by epidemiological data.
The recommended compounds—TXA, kojic acid, and niacinamide—represent a clinically validated triad for treating melasma and post-inflammatory hyperpigmentation (PIH). Tranexamic acid modulates the plasminogen/plasmin pathway to halt melanocyte stimulation, while niacinamide disrupts melanosome transfer. The transcript correctly identifies viable biochemical targets but wraps them in commercial sponsorship and accelerated timelines. For patients seeking longevity-focused skin health, these agents are efficacious but require sustained, long-term application combined with rigorous UV prophylaxis.
II. Insight Bullets
- Accumulated ultraviolet (UV) exposure is the primary driver of extrinsic skin aging, accounting for an estimated 80% to 90% of visible facial aging (dyschromia, elastosis).
- Kojic acid is a naturally occurring chelation agent that directly inhibits tyrosinase, the rate-limiting enzyme in melanin synthesis.
- The claim that kojic acid works “the very first time” is physiologically invalid; inhibiting melanogenesis requires one to two epidermal turnover cycles (4–8 weeks) for visible clinical endpoints.
- Tranexamic acid (TXA) is a synthetic derivative of the amino acid lysine, traditionally used as an antifibrinolytic, which has strong Level A evidence for melasma treatment.
- Topically applied TXA prevents UV-induced plasmin activity in keratinocytes, subsequently blocking the release of melanocyte-stimulating inflammatory mediators like arachidonic acid and prostaglandins.
- Niacinamide (Vitamin B3) does not primarily act by breaking down melanin or enhancing acid absorption; its primary depigmenting mechanism is the inhibition of melanosome transfer from melanocytes to surrounding keratinocytes.
- Licorice root extract contains the active compound glabridin, which has demonstrated in vitro capability to inhibit tyrosinase activity and decrease reactive oxygen species (ROS) production.
- OTC cosmetic formulations often lack standardized dosing and stability data, making clinical efficacy highly variable compared to prescription-grade compounds.
- The speaker’s regimen lacks the absolute requisite baseline therapy for any hyperpigmentation protocol: broad-spectrum, high-SPF daily sunscreen. Treating dyschromia without UV blockade is clinically futile.
- Plant-derived antioxidants (e.g., prickly pear, brown algae) offer adjunctive barrier support and ROS neutralization, but lack Level A evidence as primary standalone depigmenting agents.
- Retinoids, the clinical gold standard for photoaging and cellular turnover, are notably absent from the speaker’s protocol.
III. Adversarial Claims & Evidence Table
| Claim from Video | Speaker’s Evidence | Scientific Reality (Current Data) | Evidence Grade (A-E) | Verdict |
|---|---|---|---|---|
| 80% of skin aging is from sun damage. | None cited (stated as fact). | Epidemiological and histological data confirm UV radiation drives 80–90% of visible extrinsic aging (photoaging). Flament et al., 2013 | Level C (Large Observational) | Strong Support |
| Kojic acid works quickly, sometimes the “first time you use it.” | Anecdotal observation. | Tyrosinase inhibitors only prevent new melanin formation. Existing melanin must be shed via natural epidermal desquamation (~28 days). Immediate effects are cosmetic illusions (e.g., hydration, formulation optics). Saeedi et al., 2019 | Level E (Expert Opinion) | Unsupported |
| Tranexamic acid (TXA) manages future melanin cell production and works on old scars. | None cited. | Validated. TXA inhibits the plasminogen/plasmin pathway, reducing melanogenesis. Highly effective for melasma. Wang et al., 2022 | Level A (Meta-analysis) | Strong Support |
| Niacinamide helps other acids absorb deeper. | None cited. | Niacinamide improves skin barrier function (ceramide synthesis) but is primarily a melanosome transfer inhibitor. It does not act as a primary chemical penetration enhancer for acids. Navarrete-Solís et al., 2011 | Level B (RCT) | Speculative (for absorption claim) |
| Prickly pear and algae extracts super-hydrate skin and reverse premature cell death. | None cited. | These botanicals provide antioxidant (ROS scavenging) and humectant properties, improving temporary barrier function, but do not “reverse” apoptotic cell death. Guil-Guerrero et al., 2024 | Level D (Pre-clinical) | Plausible (for hydration) |
IV. Actionable Protocol (Prioritized)
High Confidence Tier (Protocols backed by Level A/B evidence)
- The Depigmentation Triad: For clinical reduction of melasma and post-inflammatory hyperpigmentation, utilize a regimen containing 3-5% Niacinamide (melanosome transfer inhibitor), 2-5% Topical Tranexamic Acid (melanogenesis cascade inhibitor), and 1-2% Kojic Acid (tyrosinase inhibitor). Apply uniformly 1-2 times daily.
- Mandatory UV Prophylaxis: No topical tyrosinase inhibitor will function without concurrent daily application of broad-spectrum SPF 30+ (preferably containing zinc oxide or iron oxides to block visible light, which heavily exacerbates melasma).
Experimental Tier (Level C/D evidence with acceptable safety margins)
- Botanical Antioxidant Adjuncts: The integration of licorice root extract (glabridin) or algae extracts can be used to augment barrier hydration and provide exogenous ROS defense against environmental stressors. These are safe but secondary to the primary active pharmaceutical ingredients.
Red Flag Zone (Claims debunked or lacking safety data)
- “Overnight” Depigmentation: Reject any protocol claiming immediate or “first-use” reduction in hyperpigmentation. Products achieving this are utilizing temporary optical diffusers (mica, titanium dioxide) or are chemically unstable.
- Unbuffered Acid Layering: Proceed with caution when layering multiple OTC acids. Kojic acid is a known sensitizer. Aggressive application without barrier support can trigger contact dermatitis, ironically resulting in worse post-inflammatory hyperpigmentation.
V. Technical Mechanism Breakdown
- Ultraviolet (UV) Induced Melanogenesis: UV radiation generates reactive oxygen species (ROS) in keratinocytes, upregulating p53 and inducing the transcription of pro-opiomelanocortin (POMC). POMC is cleaved into alpha-melanocyte-stimulating hormone (alpha-MSH), which binds to the melanocortin 1 receptor (MC1R) on adjacent melanocytes, initiating the melanin production cascade.
- Tyrosinase Inhibition (Kojic Acid): Kojic acid (5-hydroxy-2-(hydroxymethyl)-4H-pyran-4-one) acts primarily by chelating copper ions at the active site of tyrosinase. By binding the copper, it prevents the enzyme from catalyzing the hydroxylation of L-tyrosine to L-DOPA and the subsequent oxidation of L-DOPA to dopaquinone, effectively stalling eumelanin and pheomelanin synthesis.
- Plasminogen Pathway Modulation (Tranexamic Acid): UV light activates plasminogen activator in keratinocytes, increasing plasmin. Plasmin increases intracellular arachidonic acid and prostaglandins, which act as melanogenic stimulators. Tranexamic acid acts as a synthetic lysine analog; it reversibly binds to the lysine-binding sites on plasminogen, blocking its conversion to plasmin and short-circuiting this inflammatory melanogenic loop.
- Melanosome Transfer Inhibition (Niacinamide): Once melanin is synthesized within the melanocyte, it is packaged into organelles called melanosomes. These melanosomes travel along dendrites and are phagocytosed by adjacent keratinocytes to cap and protect the nuclear DNA. Niacinamide specifically disrupts the PAR-2 (Protease-Activated Receptor 2) pathway, reducing the transfer of melanosomes to the keratinocytes by up to 68% in vitro, thereby leaving the upper epidermal layers less pigmented.
Topical Compounds for Skin Health and Dyschromia Management
- Kojic Acid: A chelation agent that directly inhibits tyrosinase by binding copper at the enzyme’s active site, effectively stalling the synthesis of eumelanin and pheomelanin.
- Tranexamic Acid (TXA): A synthetic lysine analog that reversibly blocks the plasminogen/plasmin pathway, halting the UV-induced inflammatory cascade that stimulates melanogenesis.
- Niacinamide (Vitamin B3): Disrupts the PAR-2 (Protease-Activated Receptor 2) pathway to inhibit the transfer of pigment-containing melanosomes from melanocytes to keratinocytes; upregulates ceramide synthesis for barrier support.
- Licorice Root Extract (Glabridin): A botanical agent demonstrating in vitro capacity to inhibit tyrosinase activity and neutralize reactive oxygen species (ROS).
- Prickly Pear Extract: A botanical antioxidant utilized primarily for ROS scavenging and mitigation of oxidative stress.
- Algae Extracts (Green and Brown): Marine-derived humectants that improve epidermal hydration and support temporary barrier integrity.
- Zinc Oxide & Iron Oxides: Mineral filters providing broad-spectrum UV and visible light blockade, serving as the mandatory prophylactic foundation for any depigmentation protocol.
- Retinoids: Vitamin A derivatives acting as the clinical gold standard for accelerating cellular turnover, downregulating matrix metalloproteinases (MMPs), and structurally reversing photoaging.
Interestingly, the summary didn’t mention Hydroquinone cream, which is the strongest anti-pigmentation treatment, as far as I know.
It was found that hydroquinone users had higher rates of leukemia and lymphoma, possibly due to DNA damage. This is associational, not proof of causation, but it raises concern. U.S. FDA removed OTC hydroquinone due to safety concerns, including possible cancer risk, but did not declare it carcinogenic.
EU, Australia, Japan banned OTC hydroquinone out of caution.
Good point, thanks for raising it. I found the study here:
https://www.jidonline.org/article/S0022-202X(23)00491-8/fulltext
As you said, it’s quite a strong association but it comes from a database search so doesn’t show causation. Still, it’s a big increase, and there’s a plausible mechanism.
I believe topical hydroquinone is used for fairly short periods of time to treat dark patches etc. It’s not something you’d really use in a typical beauty regime. If I had severe melasma on my face or something, I’d still consider it.
I purchased a bunch of hydroquinone prescription cream from India and have been trying it out. If you follow the strict guidelines on use I think it’s fine. It seems very effective. You need to limit the square inches of skin you use it on, and the duration (I think you want to use it in 3 month pulses, if I remember correctly). Price is a few dollars a tube. Probably much more effective than the over the counter nutraceutical topical formulations: Adapalene (Differin) Report / Skincare Benefits - #21 by RapAdmin
Full list of products, prices and video on hydroquinone here: How to Reverse Skin Aging (2022 to 2024) - #447 by RapAdmin
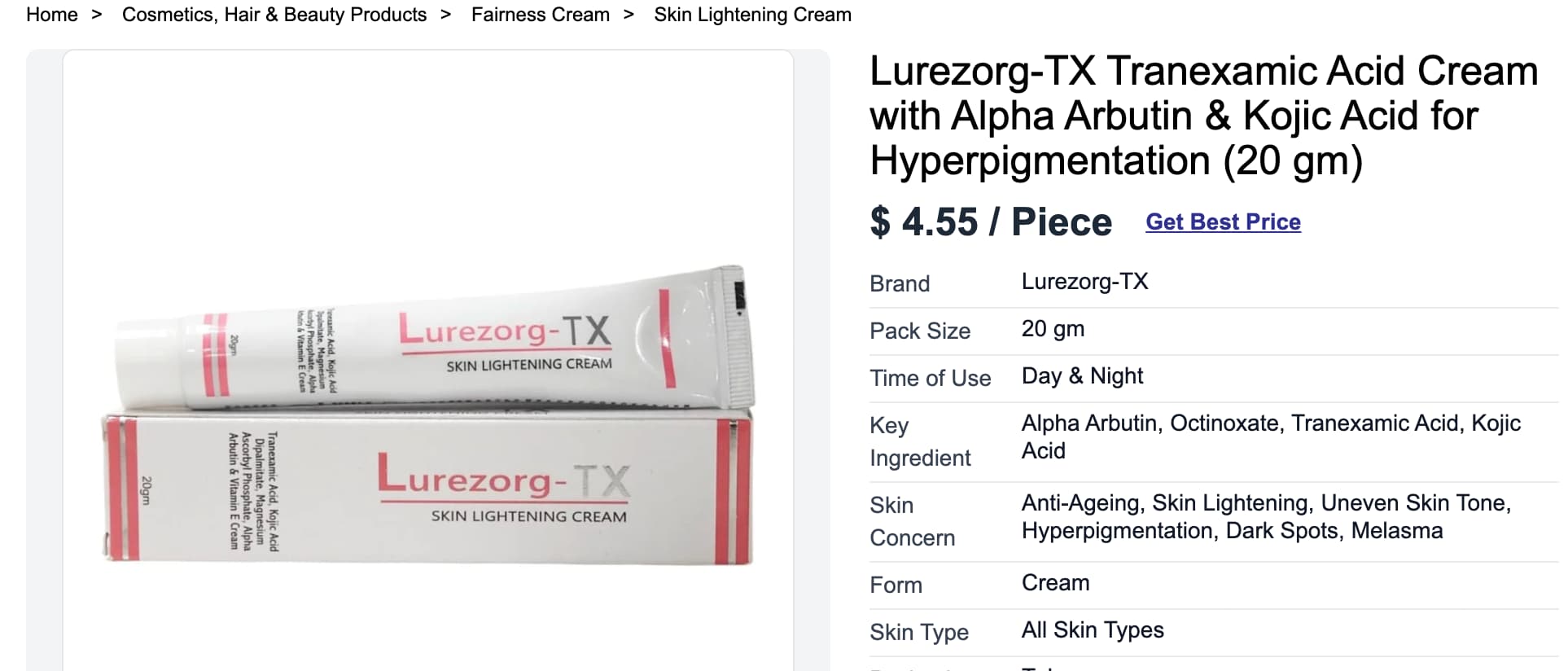
In an ideal world you might use combinations of the products; many of the products seem to be mixed this way with hydroquinone / Kojic acid, etc. Like the one below, listed on IndiaMart:
Just saw this in my google news feed:
Part of the problem is that “dark spots” is a vague classification that is used to describe several biologically distinct conditions, and they don’t all respond to the same treatments. How hyperpigmentation looks and behaves depends on what part of the body it’s on — as does how it’s perceived. Research on visual aging has found that uneven facial pigmentation plays a significant role in how old we appear: In one widely cited study published in the Journal of the American Academy of Dermatology , women with hyperpigmentation on their cheeks were perceived to be up to 20 years older than their actual age.
…
What ingredients help fade dark spots at home?
Belkin recommends looking for brightening ingredients that interrupt pigment production, such as vitamin C, niacinamide, kojic acid, n-acetylglucosamine, azelaic acid, tranexamic acid, or licorice-root extract. Gentle chemical exfoliants like glycolic, lactic, or mandelic acids can also help by speeding up cell turnover so pigmented cells shed more quickly. Retinol and bakuchiol also work in this way.
I went and did a consult for CO2 laser therapy and microneedling. I’m going to do them together as soon as I find 10 days in my schedule where I can just hide and not be seen since the recovery is brutal to say the least. CO2 is a hell of a treatment from what it looks like though
My wife has done the CO2 laser, and yeah the first 7 days or so afterwards were rough. Looks like a bad sunburn, and if they focus on any spots, they go super red. Once that faded, I would say she looked back to normal for the next ~2 weeks or so. But by 1 month she definitely looked better - skin much smoother, brighter, plumper.
Only very brave ppl can go through such skin abuse in hope of good results that hopefully would last. I would never do it for myself. Could you please update us again in the same in 6-12 months? Interested in the final outcome.
I had CO2 and not sure it made a noticeable difference.
My friend had it done to the point of looking like she was in a fire, and she was very pleased with her results.
If you go gentle or fractional you have much better recovery but the results are subtle and you’d need a few rounds spaced months apart to really make a difference. If you go meatgrinder level like your friend, then the recovery is brutal and you also risk infections or other complications. If you dodge those bullets then you likely have a much more impressive result.
I haven’t done it myself and will not consider it because I’ve got other tools in the arsenal for my needs that I much prefer. But IF I wanted CO2-like results, I’d probably do a series of chemical peels instead (high % TCA). They work very similarly and peels can be self administered at a tiny fraction of the cost. CO2 laser isn’t something I’d dabble into self administration or want to purchase the device.
The only exception is eyelids — you can’t do chemical peels on those boys but you can laser the skin off of them … by a properly trained technician or preferably cosmetic dermatologist with eye shields / guards on.
She actually did it a few years ago. It’s just really difficult to say whether it lasted or not, because there are other factors at play. She did it because she was feeling a bit “rough” after we were done having kids. We both think her skin got a lot better, and she still looks great now - but at the same time, the youngest kid has grown up, sleeps through the night etc, plus all the other skincare interventions (LED face masks, OneSkin a few months ago).
^ In related news a really cool paper was just published in Cell by a team at Harvard. They showed that embryonic skin is capable of regenerating full-thickness skin injuries, due to the absence of a specific fibroblast subpopulation. These “postnatal wound-specific” fibroblasts inhibit regeneration of multiple lineages/secondary structures by driving excessive innervation within the wound. Blocking Cxcl12 signaling within these fibroblasts, or blocking neurotransmitter release with Botox, are both sufficient to drive a regenerative wound healing response instead.
This suggests that controlled skin damage (e.g microneedling) would show enhanced recovery in the presence of Botox. I searched for a bit and found quite a few reports on people combining Botox with microneedling, but the vast majority of them are doing microneedling first. According to this, you’d want the Botox simultaneously, so it can suppress the neural activity which in turn suppresses regeneration. You might also want a microneedling device which can deliver Botox directly to the dermal layer of the wounds.
The below image was an individual who survived scalping as a child. Perhaps Botox and/or an antagonist of CXCR4 (the receptor through which CXCR4 signals) and he’d still be an NW < VII.
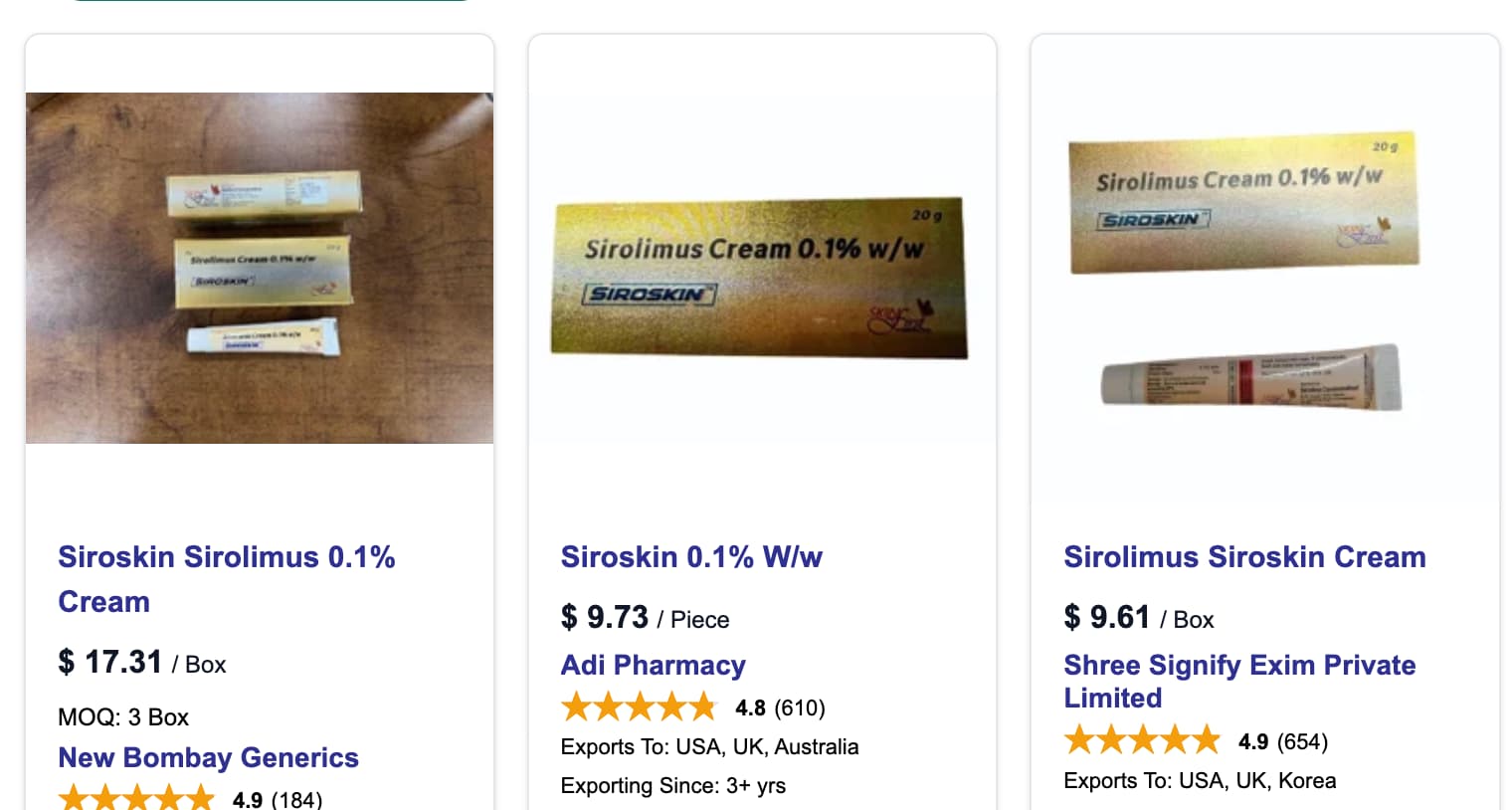
On Indiamart you can now find topical rapamycin cream, 0.1%, under the generic brand name Siroskin.
Great news! I’ll definitely be trying that now.
Does anyone combine it with Tretinoin or is it better to use them on alternating days? How often should someone be using the Rapamycin cream?
Skin cells remember inflammation for life. Here’s why
Skin remembers. That scar above your eye from when you fell at age 6. That freckle from the summer you turned 13. Our skin is a repository of moments from our lives, and now scientists have found it really does remember. For people with inflammatory skin conditions such as psoriasis, the skin’s memory manifests in flare-ups in the same spots over and over. And now scientists think they know precisely why this happens.
In a new study in mice published on Thursday in Science, researchers showed how skin cells inherit patterns of gene expression every time they regenerate. The team found not only that successive generations of skin cells maintain the memory of their DNA’s structure but also that the cells inherit chemical modifications to the DNA called epigenetic marks, which can turn on or off, or turn certain genes up and down in a process called gene expression.
“People knew that stem cells had the ability to change their behavior and remember, but they didn’t know if it was through this epigenetic mechanism,” says Shruti Naik, a molecular biologist at the University of Maryland, College Park, who has previously worked with the study’s senior author, Elaine Fuchs, but was not involved in the new research. “And I think what this paper does is definitively demonstrate that it’s through marking of DNA … that it allows that stem cell to now behave differently moving forward.”
Skin stem cell memory can be beneficial: if you get a cut, for example, your skin will heal faster in that place if it is injured again because the cells remember the experience. But that becomes problematic in conditions like psoriasis, for which the memory of a flare-up can make the tissue overly sensitive to environmental triggers such as stress, leading to chronic inflammation.
“Your DNA can remember, far longer than we appreciated, a past injury,” says Dana Pe’er, a co-author of the study and chair of the Computational and Systems Biology Program at the Sloan Kettering Institute. “It’s a double-edged sword.”
Read the full story: Skin cells remember inflammation for life. Here’s why (Scientific American)
This is why human life is limited to 115 to 120 years
Among other factors