The transition from reactionary sick-care to proactive geroscience requires a fundamental shift in public understanding and healthcare infrastructure. As global populations age, healthcare systems face unsustainable economic burdens from age-related chronic diseases. A recent nationwide survey conducted by the National University of Singapore evaluated public literacy on longevity concepts and the baseline demand for Healthy Longevity Medicine (HLM) clinics in Singapore. The findings reveal a significant “healthspan knowledge gap” that public health officials and biotech developers must actively address before scaling advanced longevity interventions across populations.
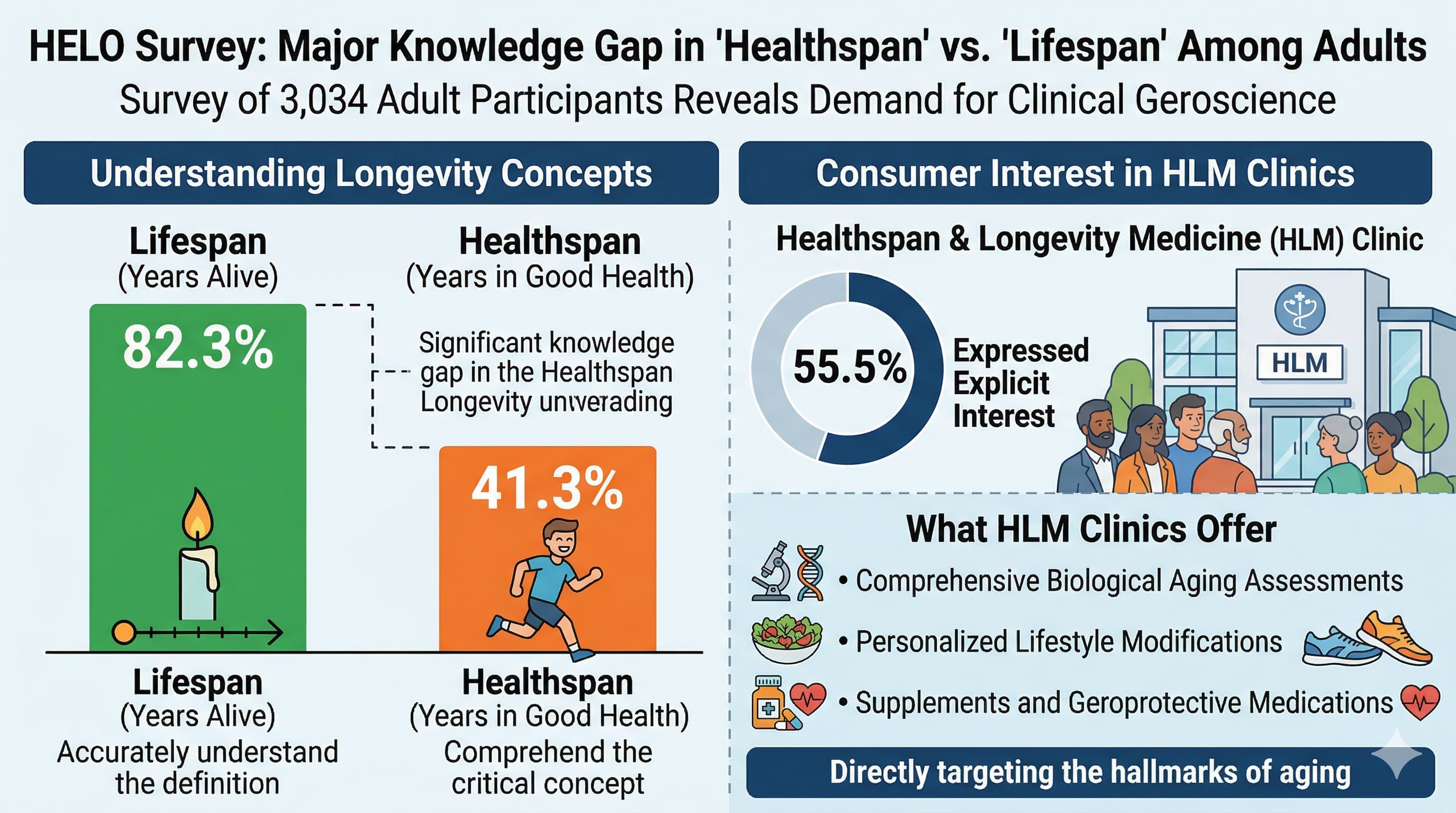
The cross-sectional HELO survey involved 3,034 adult participants and demonstrated that while the vast majority (82.3%) accurately understand the definition of “lifespan” (years alive), less than half (41.3%) comprehend the critical concept of “healthspan”—the period of life spent in good health. Despite this lack of specific terminology, the data indicates robust consumer demand for clinical geroscience. Over half of the cohort (55.5%) expressed explicit interest in attending an HLM clinic. These specialized clinics are designed to offer comprehensive biological aging assessments and prescribe personalized lifestyle modifications, supplements, and geroprotective medications to directly target the hallmarks of aging.
Predictors for HLM interest and healthspan literacy provide a clear demographic target for early adopters of longevity therapies. Younger age, male gender, higher education, and higher income levels were significantly associated with better knowledge and greater clinical interest. Furthermore, individuals already engaged in proactive health behaviors—such as taking supplements, exercising frequently, and paying out-of-pocket for annual health screenings—were the most likely to understand healthspan and seek out HLM services. Curiously, moderate alcohol consumption (1 to 7 drinks per week) also correlated with higher interest and knowledge compared to total abstinence, a finding the authors suggest may reflect higher socioeconomic status or socialization patterns rather than a biological advantage.
This data strongly suggests that the bottleneck for clinical longevity is not consumer interest, but rather conceptual education and clinical accessibility. If the biotech and public health sectors intend to translate interventions targeting fundamental aging pathways into standard clinical care, they must first standardize the definition of healthspan and close the public knowledge gap.
Source:
- Open Access Paper: Knowledge of lifespan and healthspan and interest in Healthy Longevity Medicine among the general population in Singapore: the Singapore HEalthy LOngevity (HELO) survey
- Journal: Geoscience
- Impact: The impact score of this journal is 5.4, evaluated against a typical high-end range of 0–60+ for top general science, therefore this is a Medium impact journal.