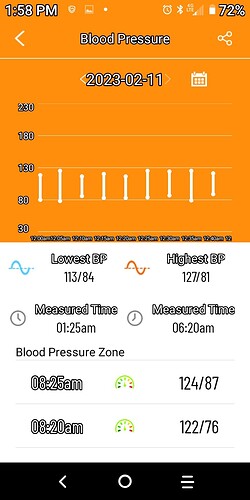
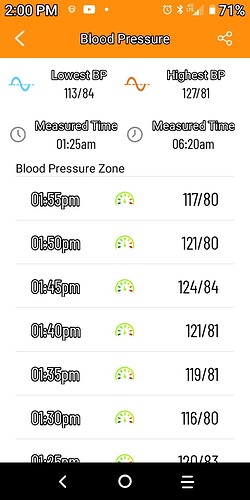
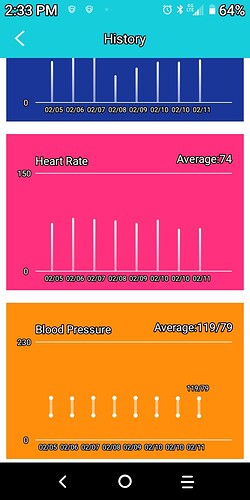
I had been taking rapamycin since August, quickly working my way up to 3mg and then staying there until over the past 6 weeks upping my dose to 6mg weekly. 2 weeks ago, I started having headaches and feeling a bit lightheaded. I stopped taking rapa the following week out of caution. The headaches and pressure and lightheadedness continued through this week along with ringing in my ears. After some googling and consulting Dr. ChatGPT I began to think this might be due to raised blood pressure. I dug out my automatic blood pressure cuff and it read 160/80! Not emergency-room level, but not at all good. And much higher than it has been for most of my life.
I am going to carefully monitor my blood pressure and stay off rapamycin at any dose for the time being. If it increases at all, I will immediately go to the doctor. If it can resolve now that I have ceased taking rapamycin, that would probably be best rather than starting treatment for something that might resolve on its own. Online sources say pressure usually resolves within 1-4 weeks. If it does not resolve or if it increases at all, I will go to the doctor.
The interaction seems to be an activation of the renin-angiotensin-aldosterone system. Here’s what our buddy ChatGPT had to say about it:
Rapamycin is known to increase the expression of the gene encoding for renin, the first enzyme in the renin-angiotensin-aldosterone system (RAAS). This increase leads to increased production of angiotensin II, which is a potent vasoconstrictor and stimulates the secretion of aldosterone. The elevated levels of angiotensin II and aldosterone result in constricted blood vessels and fluid and sodium retention, leading to increased blood pressure. Rapamycin also has direct effects on the cardiovascular system, reducing the responsiveness of blood vessels to dilating stimuli and the contractile function of the heart. The exact mechanisms of how rapamycin affects blood pressure and the RAAS are not fully understood, but the current working theory suggests that the increase in blood pressure seen with rapamycin is due to its effects on the RAAS and its direct effects on the cardiovascular system.
The exact mechanisms by which rapamycin affects the expression of the gene encoding for renin and the activation of the renin-angiotensin-aldosterone system (RAAS) are not fully understood, but it is believed to involve the mechanistic target of rapamycin (mTOR) pathway, specifically the mTORC1 complex.
I honestly don’t know if the two are related for sure, but considering that was a change and this very closely followed, I think it’s a reasonable guess.
Assuming my levels return to normal, I will consider restarting at the 3mg level and watch my blood pressure for signs of increase very closely. I’ll keep you all updated!