Your daily dose of recent SGLT2 papers:
Study funded by the UK Medical Research Council (government body): Safety and effectiveness of SGLT2-inhibitors in people with type 2 diabetes over 70: UK population-based study using an Instrumental Variable approach. Not yet peer-reviewed, but it confirms the “very low” DKA risk, even among T2D (and especially among people less than 70yo). Unfortunately, no side-by-side SGLTi comparison in the paper:
Risk of DKA was increased with SGLT2-inhibitors in those aged ≥70 (Incidence risk ratio compared to DPP4i: 3.82 [95%CI 1.12,13.03]), but not in those <70 (1.12 [95%CI 0.41,3.04]). However incidence rates with SGLT2-inhibitors in those ≥70 was low (29.6 [95%CI 29.5,29.7]) per 10000 person-years. […] DKA is a rare AE and the risk increase with SGLT2-inhibitors may be restricted to adults over 70 […] Although we found DKA risk with SGLT2-inhibitors was elevated in those over 70, incidence was very low. […] SGLT2-inhibitors in older adults are effective and do not increase risk of dehydration, falls or urinary problems in older adults with T2D. However, risk of genital infections is increased, and DKA is a rare but severe adverse event of concern, meaning baseline DKA risk should be carefully assessed before initiation of SGLT2-inhibitors."
Meta-analysis of 17 RCTs (100k+ patients): GLP-1 receptor agonists, SGLT2 inhibitors and noncardiovascular mortality in type 2 diabetes: Insights from a meta-analysis 2024. (No side-by-side SGLTi comparison either. Similar results for GLP1RA btw, so they’re also quite good.)
Compared to placebo, SGLT2i significantly reduced noncardiovascular mortality (RR = 0.90; 95%CI: 0.82–0.99; I2 = 0 %; p < 0.05) along with cardiovascular mortality (RR = 0.84; 95%CI: 0.77–0.92; I2 = 28 %; p < 0.001).
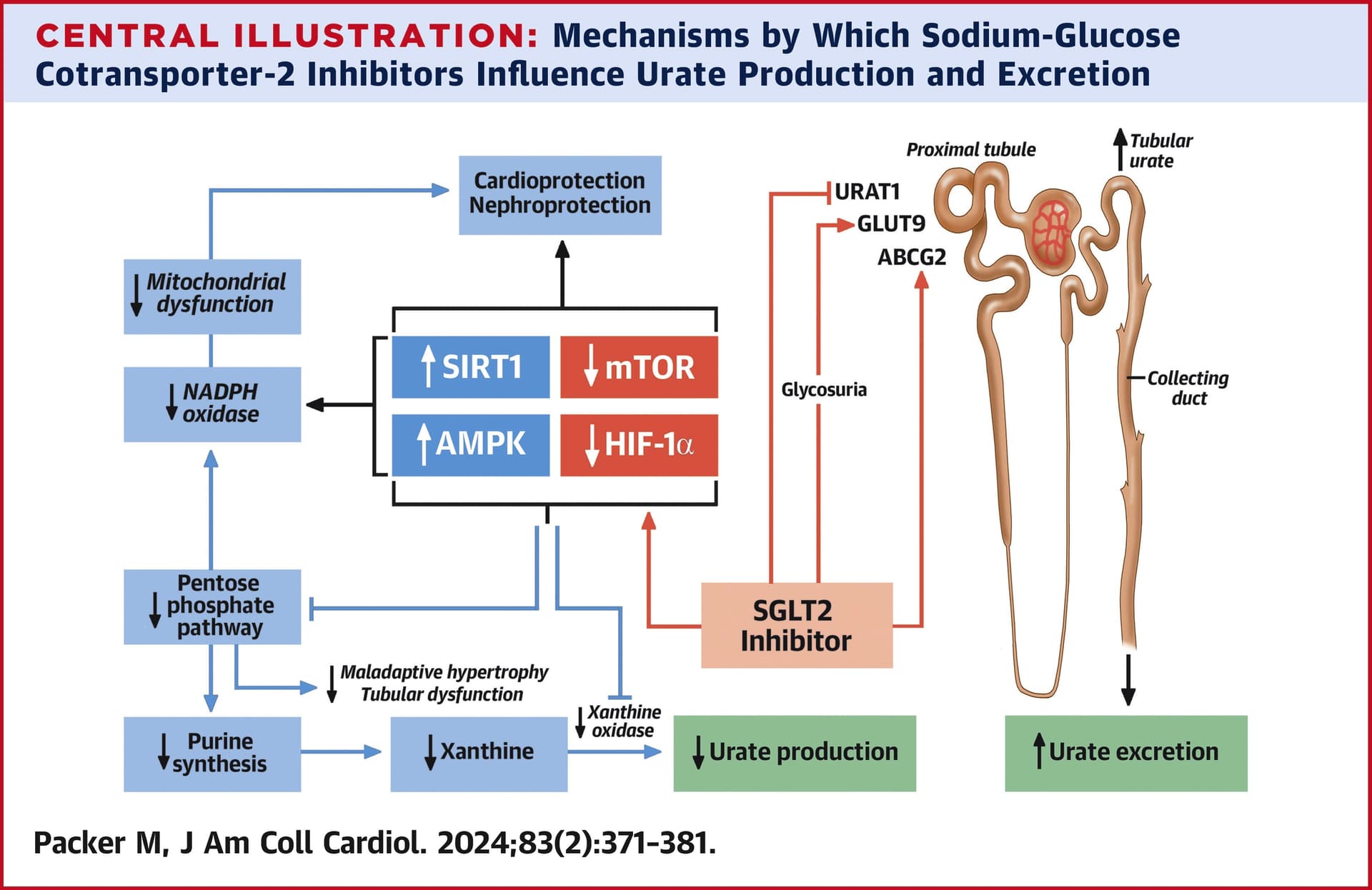
Good review in the Journal of the American College of Cardiology: Hyperuricemia and Gout Reduction by SGLT2 Inhibitors in Diabetes and Heart Failure: JACC Review Topic of the Week 2024
SGLT2 inhibitors induce a state of starvation mimicry at a molecular, cellular, and physiological level, which is characterized by glycosuria and ketogenesis and by upregulation of nutrient deprivation signaling (ie, SIRT1) and downregulation of nutrient surplus signaling (ie, mTOR and HIF-1α). […] The actions of SGLT2 inhibitors to upregulate both SIRT1 and AMPK and downregulate both mTOR and HIF-1α are seminal to their cardioprotective and nephroprotective effects.
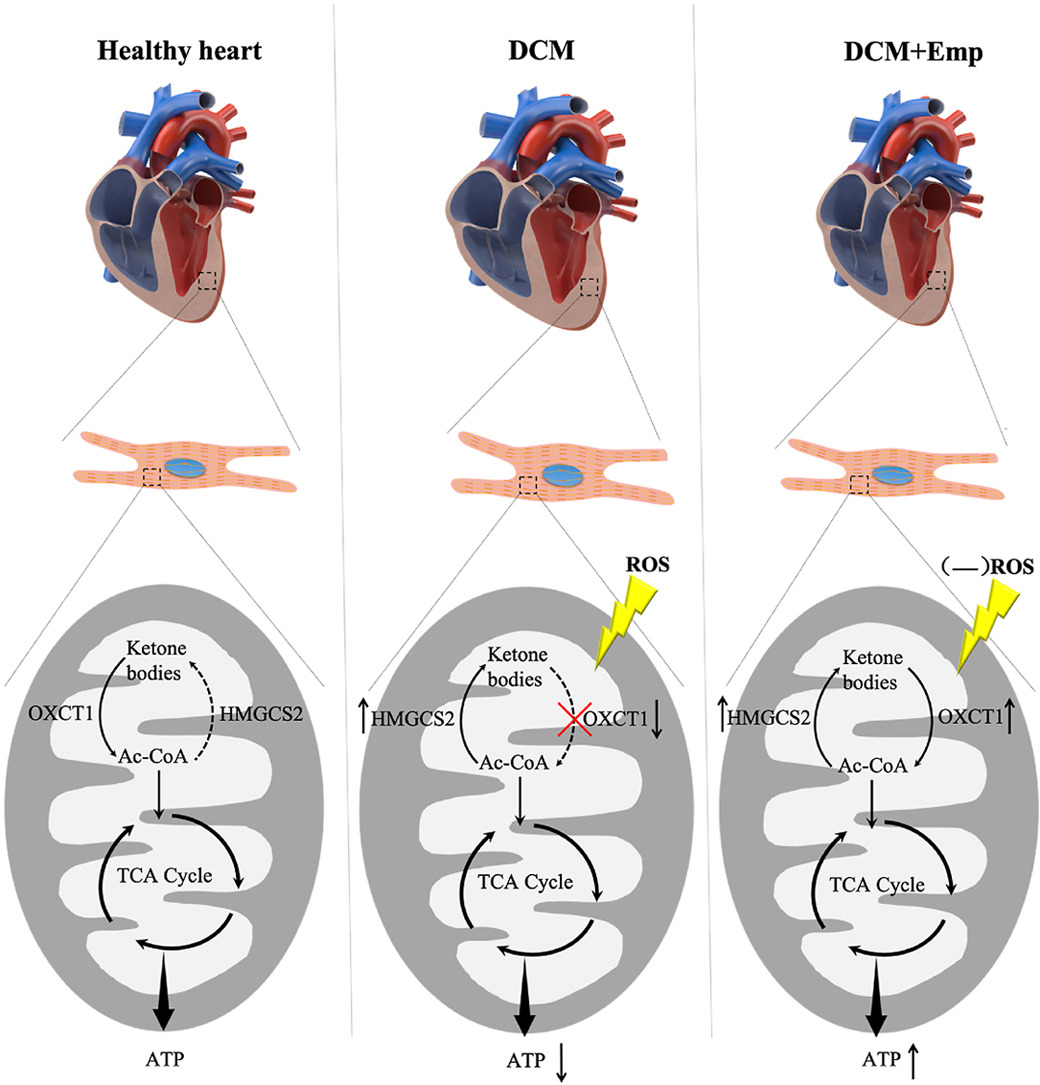
Small study trying to understand why and how SGLT2i improve outcomes: Empagliflozin Improves Vascular Insulin Sensitivity and Muscle Perfusion in Persons with Type 2 Diabetes 2024
Following empagliflozin, insulin infusion improved endothelial function (p=0.02), lowered peripheral and aortic systolic (each p<0.01), diastolic (each p<0.05), mean arterial (each p<0.01), and pulse pressures (each p<0.02), altered endothelial biomarker expression, and decreased radial artery forward and backward pressure amplitude (each p=0.02). Empagliflozin also improved insulin-mediated skeletal and cardiac muscle microvascular perfusion (each p<0.05). We conclude that empagliflozin enhances insulin’s vascular actions which could contribute to the improved cardio-renal outcomes seen with SGLT2i therapy.