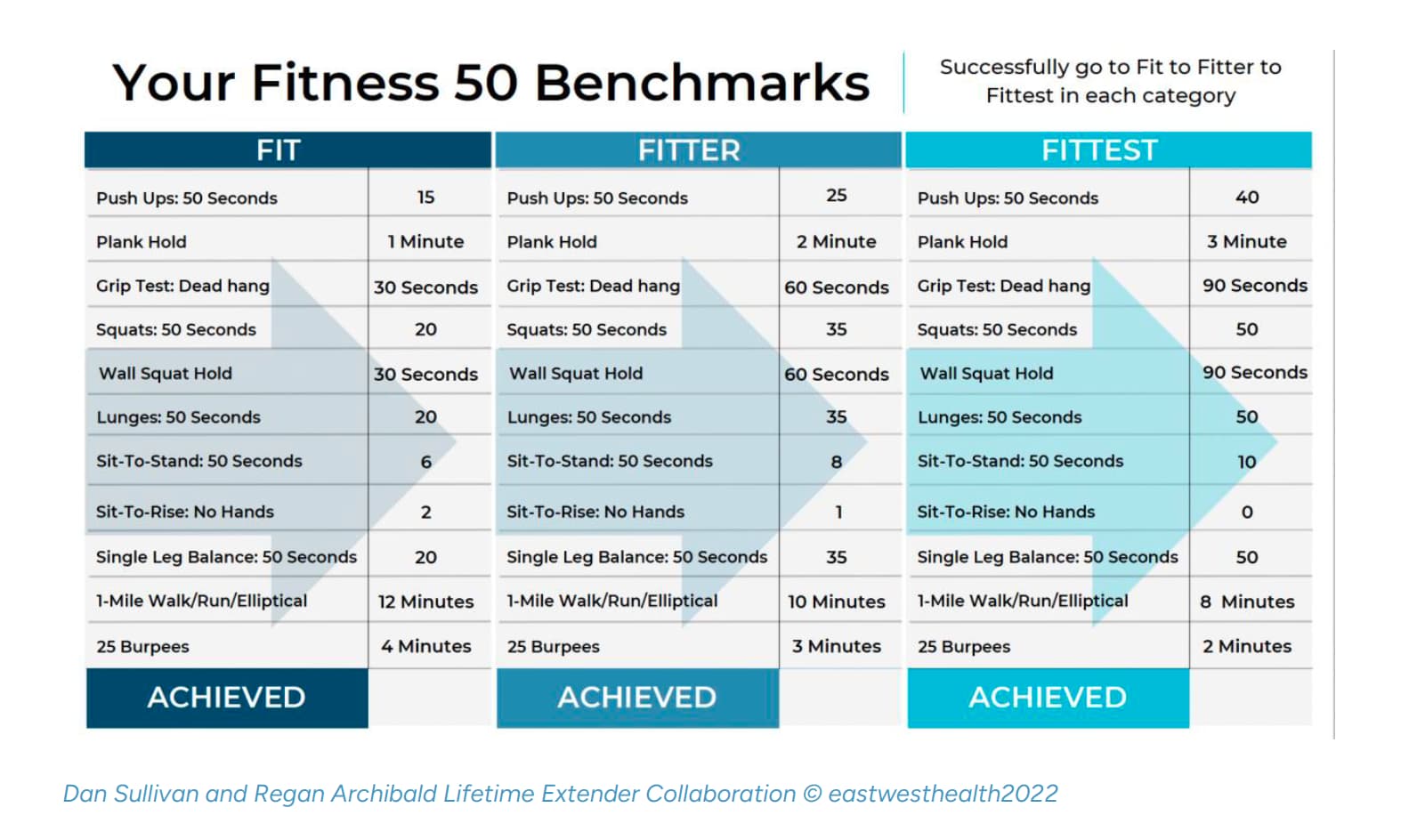
The new Outside magazine article / interview with Peter Attia has some discussion on the functional biomarkers that he uses…
VO2 max measures the amount of oxygen your muscles can utilize at peak effort. It’s the benchmark of cardiovascular fitness because it’s a picture of how well oxygen moves through your system. You can’t game the results. It has also, somewhat recently, become a useful predictor of longevity. If some fitness is good, is more better? Apparently so. Numerous studies have found that higher VO2 max scores correlate with longer life.
…
My score tops out at 41.6, which strikes me as low, but Bennett says it’s actually pretty good for a guy my age. I’m quietly thrilled to see my report sheet include the word “excellent.” Still, I’m a bit short of the Elite category, which requires hitting 50 or above. In Outlive, Attia states that he wants his clients to aim for a VO2 max score in the Elite zone for their gender but two decades younger. In my case, that would mean a score of around 53, a daunting target based on what it took to hit 41.
That seemed highly improbable, but Bennett assures me I can get there, or close. And what, I ask, might it require? Something in the range of four to six hours of Zone 2 work, plus at least one Zone 5 interval session, per week, he says.
Zone 2 is the quasi-magical aerobic threshold, where it’s possible to burn fat as fuel more than you’re burning carbohydrates. Zone 2 is the kind of effort you can sustain for a long time. Zone 2 is pretty easy. I love Zone 2.
Zone 5 training is quite hard, but it’s mercifully brief. A popular Zone 5 workout involves four minutes of maximum effort followed by four minutes of recovery, done a total of four times. One of my big takeaways from testing is realizing how these zones actually feel. What I thought was Zone 2 was probably more like Zone 3 or even 4. My easy workouts have not been easy enough, I discover, and my hard sessions are not hard enough. I’ve been trapped in the middle, a metabolic no-man’s land.
…
I’d long thought of lifting weights as essential for athletic performance, regardless of your sport, but I hadn’t considered the impact on healthy aging. Not only does preserving lean muscle deliver metabolic benefits, but it also helps keep us mobile and stable. Falls are the leading cause of death after age 65—the fifth horseman.
Not surprisingly, given my cyclist’s approach to upper-body development, I fare less well at strength. The goal for the arm hang is two minutes. That doesn’t sound like much, but it’s surprisingly difficult. I don’t even make it to one minute.
The goal for the hex-bar carry is similarly challenging: carry your body weight—in my case 186 pounds—for 60 seconds. Once again I come up short. Not to worry, Bennett tells me. With a dedicated lifting regimen, I can meet these standards as well.
…
Fitness Institute of Texas website: FITNESS INSTITUTE of TEXAS
Online Fitness Progams: Get FIT - FITNESS INSTITUTE of TEXAS
“There is no short-term fix,” Blue Zones’ s Dan Buettner told me. “If you want to live longer, you have to think about things you are going to do on a daily basis for decades.”