Google Gemini Pro AI Video Summary and Analysis
The video explores the “Lycopene Paradox” regarding cardiovascular health and atherosclerosis (plaque buildup). Initially, five observational studies suggested a strong inverse relationship: higher blood lycopene levels correlated with reduced Carotid Intima-Media Thickness (IMT), a marker of arterial plaque. However, the narrative shifts when contradictory data emerges—specifically, a large observational study showing no benefit and a Randomized Controlled Trial (RCT) showing no improvement in cardiovascular risk factors (blood pressure, lipids) after supplementation.
The analysis resolves this conflict by identifying critical flaws in the negative studies (e.g., poor dietary recall methods and short trial durations) and highlighting a pivotal, successful RCT. This successful 12-month trial demonstrated that 20 mg of Lycopene combined with 20 mg of Lutein significantly reduced arterial plaque, suggesting a synergistic effect and the necessity of long-term (1+ year) intervention. The conclusion is cautious but optimistic: while lycopene is not a “magic bullet” for everyone, it is a viable, low-risk therapeutic option for those with existing cardiovascular history, particularly when consumed via processed tomato products (paste/sauce) which offer superior bioavailability over raw tomatoes.
B. Bullet Summary
- Lycopene defined: A potent antioxidant carotenoid responsible for the red pigment in tomatoes; it neutralizes free radicals that oxidize cholesterol.
- Mechanism of action: Oxidized LDL cholesterol gets trapped in arterial walls, forming plaque. Lycopene may prevent this oxidation.
- Initial consensus: Five observational studies consistently showed that higher blood lycopene correlates with lower arterial plaque (IMT).
- The Conflict: Two subsequent studies (one observational, one RCT) found no benefit, creating a “mystery” in the data.
- Methodological flaw (Observational): The negative observational study relied on dietary recall, which correlated poorly with actual blood levels, rendering the data unreliable.
- Methodological limitation (Null RCT): The negative RCT only measured surrogate risk factors (BP, lipids) over a few months, not actual plaque regression.
- The “Winning” RCT: A specific long-term trial (Zou et al.) measured plaque directly over 12 months.
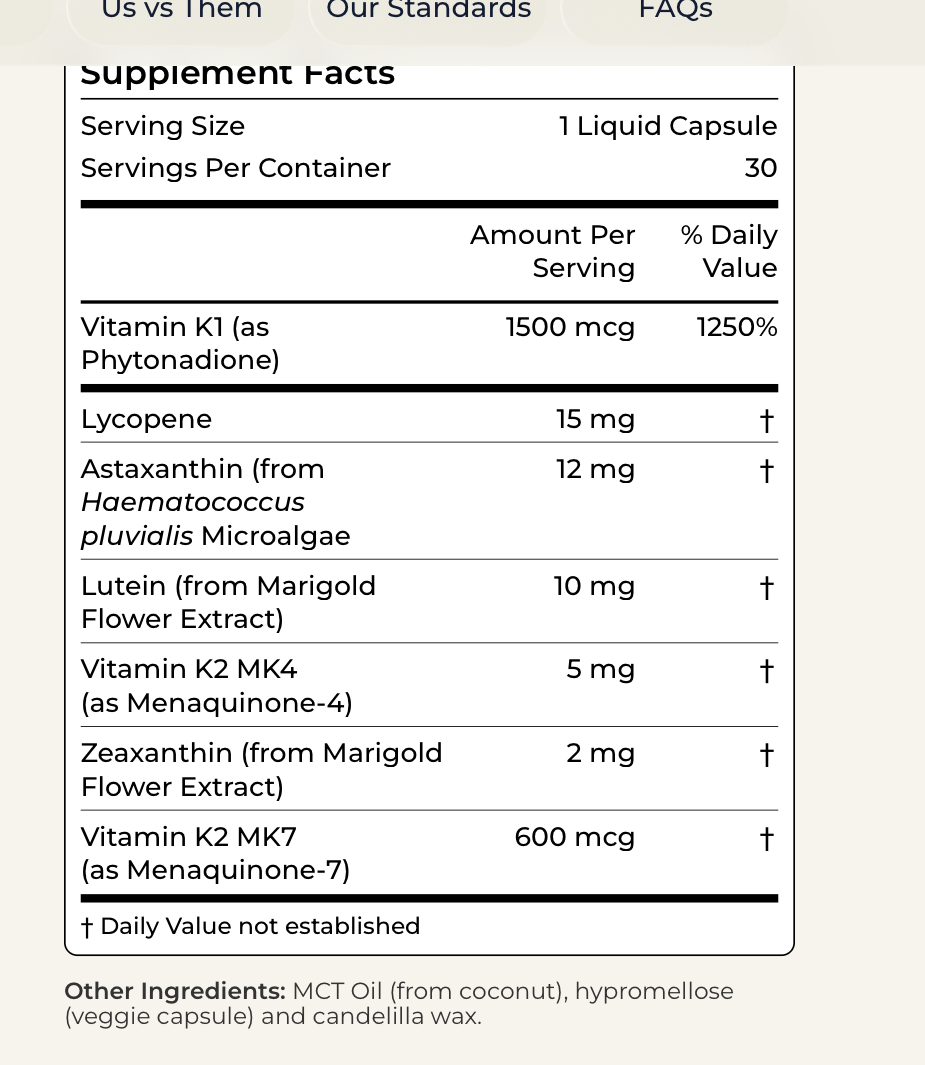
- Synergy Key: The successful trial combined 20 mg Lycopene with 20 mg Lutein.
- Results: Lutein alone reduced plaque; Lycopene + Lutein reduced it significantly more (synergistic effect).
- Duration matters: Plaque regression is slow; trials shorter than 6–12 months are likely to miss the signal.
- Dosing: The effective therapeutic dose appears to be 20 mg/day.
- Dietary Sources: Processed tomatoes (paste, sauce) are superior to raw tomatoes.
- Concentration: Raw tomatoes = 1–7 mg lycopene/100g; Tomato paste = 10–30 mg/100g.
- Bioavailability: Heating tomatoes and adding fat (oil) significantly increases absorption.
- Target Audience: Healthy individuals may not see a benefit; those with subclinical atherosclerosis (history of CVD) are the prime candidates.
- Safety: 20 mg/day is well within safe limits (observed safe level up to 75 mg/day).
D. Claims & Evidence Table (Adversarial Peer Review)
| Claim from Video | Speaker’s Evidence | Scientific Reality (Best Available Data) | Evidence Grade (A-E) | Verdict |
|---|---|---|---|---|
| “High blood lycopene is associated with less arterial plaque.” | Cites 5 observational studies (IMT vs. Blood levels). | Supported. Meta-analyses confirm inverse association between serum lycopene and Carotid Intima-Media Thickness (IMT) (e.g., Karppi et al., 2012; Cheng et al., 2017). | C (Cohort/Obs) | Strong Support |
| “Lycopene reverses/regresses plaque (Regression).” | Cites one 12-month RCT showing reduced IMT. | Plausible (Conditional). Zou et al. (2014) [Brit J Nutr] showed significant IMT reduction with 20mg Lycopene + 20mg Lutein. Lycopene alone data is weaker/mixed in other trials. | B (RCT) | Plausible (Specifically with Lutein) |
| “Short-term lycopene use doesn’t improve CV risk factors.” | Cites a “Null RCT” of short duration. | Supported. Meta-analyses (Tierney et al., 2020) find inconsistent effects on BP and lipids in short-term studies. Structural changes (plaque) take >1 year. | A (Meta-Analysis) | Strong Support |
| “Processed tomatoes (paste) have higher lycopene than raw.” | States paste has 10-30mg vs 1-7mg for raw. | Fact. Thermal processing breaks cell walls and converts trans-lycopene to the more bioavailable cis-lycopene (Gartner et al., 1997). | B (Bioavailability Trial) | Fact |
| “Lycopene + Lutein is more effective than Lutein alone.” | Cites the “Winning” RCT (Zou et al.). | Supported. Zou et al. (2014) found the combination group had the greatest reduction in IMT compared to Lutein alone or Placebo. | B (Single RCT) | Strong Support |
| “20mg is the effective dose.” | Derived from the successful RCT. | Reasonable. Most successful metabolic studies use 15-30mg. Lower doses (dietary only) often show null results in intervention trials. | B (RCT extrapolation) | Standard Protocol |
E. Actionable Insights (Pragmatic & Prioritized)
Top Tier (High Confidence & Safety)
-
The “Paste & Oil” Protocol: Do not rely on raw tomatoes. To achieve the therapeutic 20mg dose via food, consume ~100g of tomato paste or puree weekly, or divided daily.
-
Crucial Step: Always consume with a healthy fat (e.g., Extra Virgin Olive Oil) and heat it. This increases bioavailability by converting lycopene to its active cis-isomer.
-
Target Population: Prioritize this intervention if you have a family history of CVD, elevated LDL, or known subclinical atherosclerosis (calcium score > 0).
Experimental (High Upside / Low Risk)
- The “Synergy” Stack: Based on the Zou et al. trial, combine:
- Lycopene: 20 mg (softgel preferred for oil base).
- Lutein: 20 mg.
- Duration: Commit to 12 months minimum. Plaque regression is a slow biological process; checking results in 3 months is futile.
Avoid
- “Ketchup” as a Source: While processed, the high sugar/corn syrup content negates the metabolic benefits. Stick to paste, puree, or high-quality marinara.
- Expectation of Quick Fixes: Do not use Lycopene to acutely lower blood pressure or cholesterol numbers; the data does not support it as a statin replacement. It is a structural remodeling agent for the arterial wall.
H. Technical Deep-Dive: Isomerization & Plaque regression
1. The Bioavailability Barrier (Trans vs. Cis)
In raw tomatoes, lycopene exists primarily in the all-trans configuration. This linear molecule is tightly bound within the vegetable matrix (crystalloids) and is poorly absorbed by the human digestive tract.
- Thermal Processing: Heating tomatoes (as done in paste/sauce production) induces isomerization, converting the molecule to the cis-lycopene shape (bent structure).
- Mechanism: Cis-lycopene is significantly more soluble in bile acid micelles and is transported more efficiently into chylomicrons. This explains why the video emphasizes paste over raw fruit.
2. Mechanism of Plaque Stabilization
The video touches on “Anti-oxidation,” but the specific mechanism involves the Oxidative Modification Hypothesis of atherosclerosis:
- LDL Infiltration: LDL particles enter the sub-endothelial space.
- Oxidation: If antioxidants are scarce, Reactive Oxygen Species (ROS) oxidize the LDL (oxLDL).
- Foam Cell Formation: Macrophages scavenge oxLDL via unregulated scavenger receptors (CD36/SR-A), becoming lipid-laden “foam cells”—the core of the plaque.
- Lycopene’s Role: As a highly lipophilic antioxidant, lycopene integrates into the LDL particle itself. It acts as a sacrificial anode, neutralizing ROS before they can oxidize the LDL cholesterol esters, thereby preventing the foam cell cascade. The synergy with Lutein is likely due to Lutein’s varying polarity, allowing it to protect the lipoprotein surface while Lycopene protects the lipid core.