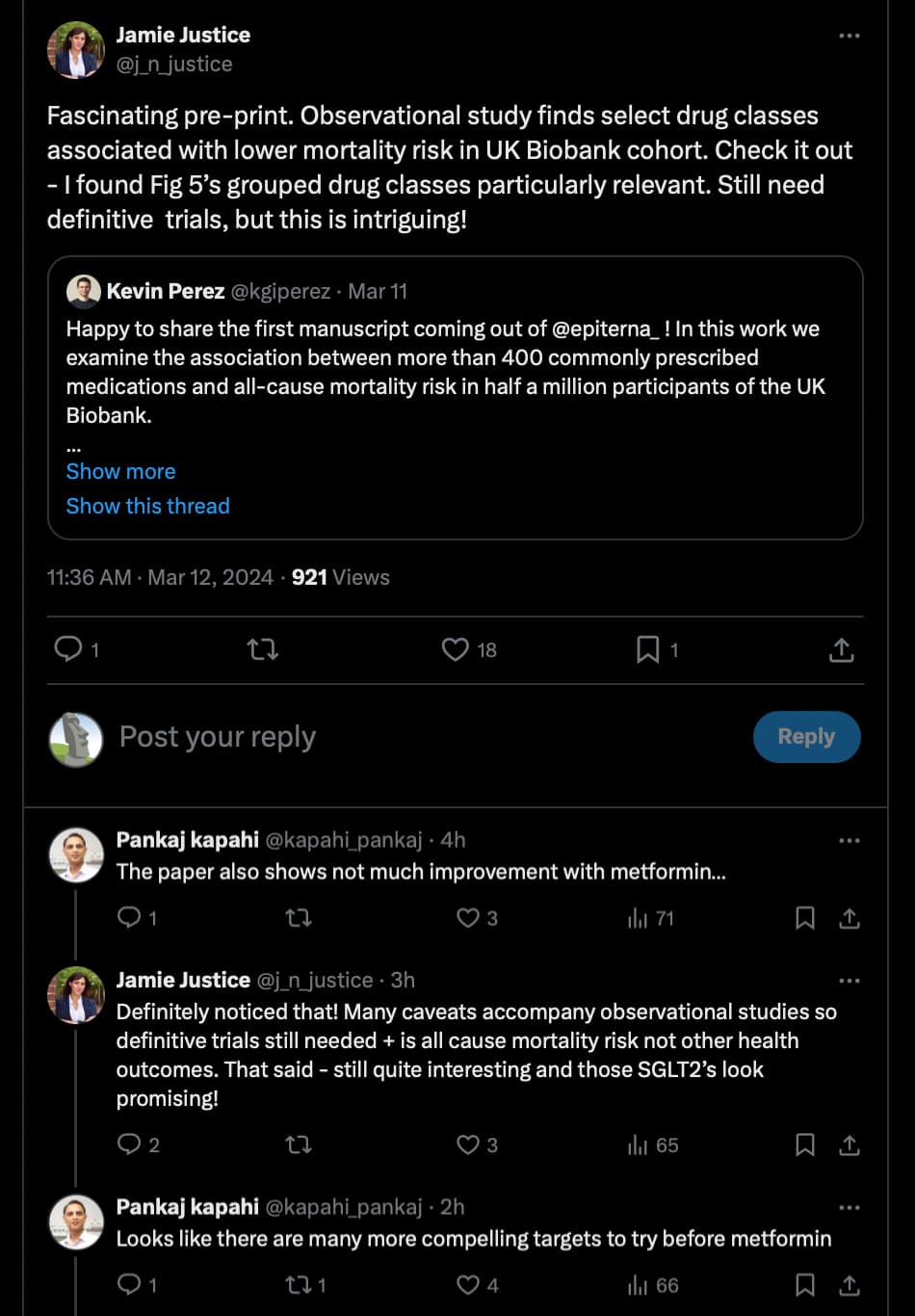
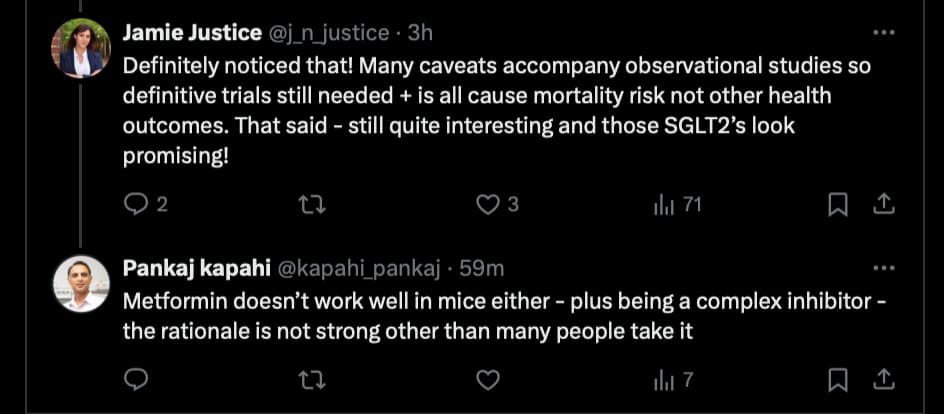
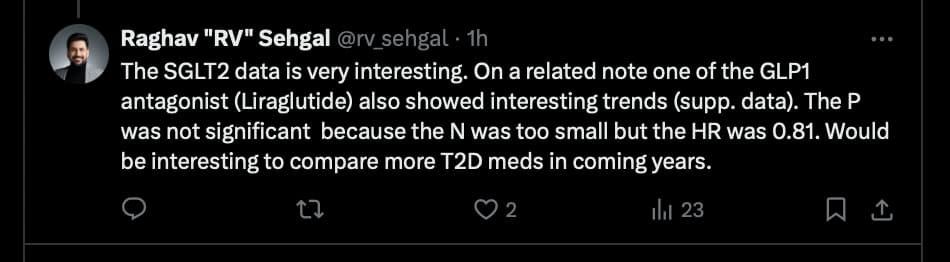
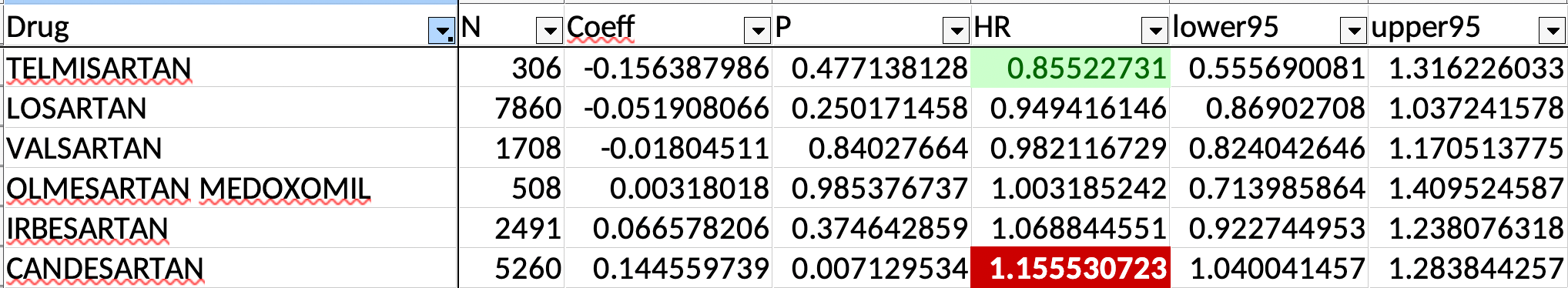
I’m always so confused about oestrogen. It seems like such a double-edged sword to me, but likely since I am not well-versed enough in the topic.
(At least in some situations, in some tissues) transdermally applied oestrogen stimulates mTOR, such as in vaginal tissues but also in liver tissues it increases IGF-1 levels and mTOR, and systemically. And in caloric restriction mTOR of course is suppressed systemically (to trigger autophagy) and LH, FSH and oestrogen levels tend to drop. That makes me wonder if taking oestrogen as a woman is really likely to increase lifespan?
Publications suggest oral versus transdermal oestrogen have different effects. Transdermal oestrogen would apparently increase circulating IGF-1 (as it bypasses first-pass metabolism) and activate mTOR, whereas that would not be the case for oral oestrogen. In fact some research suggests oral oestrogen decreases systemic mTOR. But oral oestrogen of course isn’t as effective in reducing for example bone loss in menopausal women or vaginal atrophy - osteoblast activation and vaginal wall ‘repairment’ requires cell proliferation and mTOR activation after all.
I’d love to hear a better informed opinion on this. Unfortunately GPT seems to give me different answers on different days, and the sources I ask it to include in its answers are commonly random studies that have nothing to do with the citations it made up.
https://www.nature.com/articles/s41419-022-05293-8
“The mouse vaginal epithelium cyclically exhibits cell proliferation and differentiation in response to estrogen. Estrogen acts as an activator of mTOR signaling but its role in vaginal epithelial homeostasis is unknown. We analyzed reproductive tract-specific Rptor or Rictor conditional knockout mice to reveal the role of mTOR signaling in estrogen-dependent vaginal epithelial cell proliferation and differentiation. Loss of Rptor but not Rictor in the vagina resulted in an aberrant proliferation of epithelial cells and failure of keratinized differentiation. As gene expression analysis indicated, several estrogen-mediated genes, including Pgr and Ereg (EGF-like growth factor) were not induced by estrogen in Rptor cKO mouse vagina. Moreover, supplementation of EREG could activate the proliferation and survival of vaginal epithelial cells through YAP1 in the absence of Rptor. Thus, mTORC1 signaling integrates estrogen and growth factor signaling to mediate vaginal epithelial cell proliferation and differentiation, providing new insights into vaginal atrophy treatment for post-menopausal women.”
https://pubmed.ncbi.nlm.nih.gov/1991807/
“Oral EE treatment increased mean 24-h serum GH (2.0 +/- 0.4 to 7.0 +/- 0.6 mIU/L, P less than 0.0005) and mean pulse amplitude (5.3 +/- 1.2 to 11.2 +/- 2.5 mIU/L, P less than 0.01) but significantly reduced circulating IGF-I (0.70 +/- 0.09 to 0.47 +/- 0.04 U/mL, P less than 0.02) levels. Oral EE increased the percent specific binding of [125I]GH (22.0 +/- 1.6 to 32.0 +/- 1.9%, P less than 0.0005), however the derived mean 24-h free serum GH concentrations were significantly higher (P less than 0.0005) after treatment. By contrast, transdermal E2 administration, which restored circulating E2 concentrations to the midfollicular range, increased circulating IGF-I (0.86 +/- 0.15 to 1.10 +/- 0.14 U/mL, P less than 0.005) to levels that were not significantly different from those of premenopausal women (1.41 +/- 0.21 U/mL). This was not accompanied by changes in 24-h GH secretion or the percent specific binding of [125I]GH in serum. The route of administration is a major determinant of the effects of exogenous estrogens on the GH/IGF-I axis. Oral estrogen administration inhibits hepatic IGF-I synthesis and increases GH secretion through reduced feedback inhibition. Reduced GH secretion in the menopause is not explained by estrogen deficiency since GH secretion is not restored by the attainment of physiological E2 concentrations using the transdermal route. The contrasting route dependent IGF-I responses have important implications for the long-term benefit of hormone replacement therapy in the menopause.”
https://pubmed.ncbi.nlm.nih.gov/25001019/
“After 10 weeks of CR or high-fat diet, ovarian follicles at different developmental stages were examined by histological analysis. Plasma levels of luteinizing hormone (LH), follicle-stimulating hormone (FSH), and estrogen (ESG) were measured, and the levels of mammalian target of rapamycin (mTOR), p70S6 kinase (p70S6K), and phosphorylated p70S6K in the ovary were detected by Western blot. The results showed that the reserve of follicle pool in CR rats was increased, accompanied by decreased level of phosphorylated p70S6K in the ovary, and decreased serum LH, FSH, and ESG levels. Taken together, these results suggest that CR may suppress ovarian follicular development and enhance the follicle pool reserve by inhibiting mTOR signaling.”
(That is all besides the ITP study that showed 17-alpha-estradiol significantly increased the median lifespan of male mice but had no significant effect on females. Albeit there is a lot to discuss about that also).