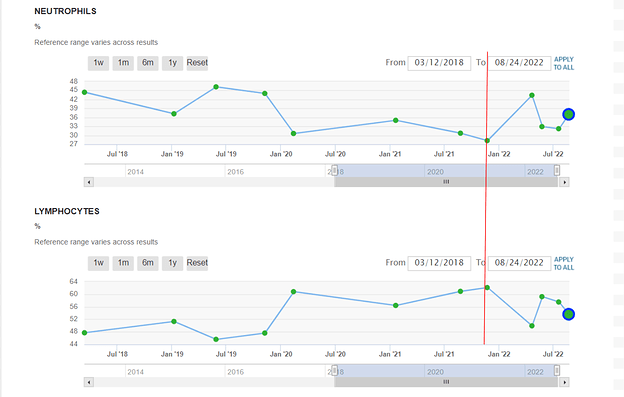
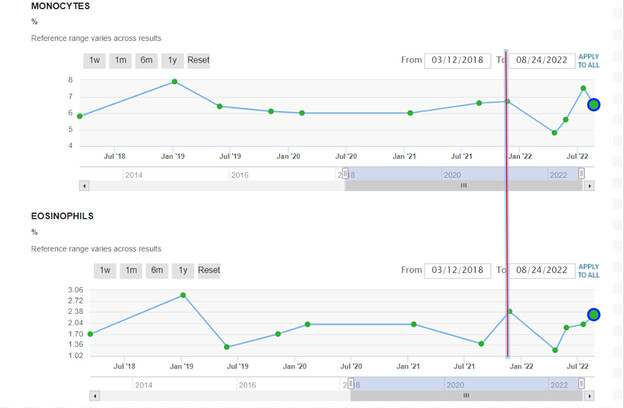
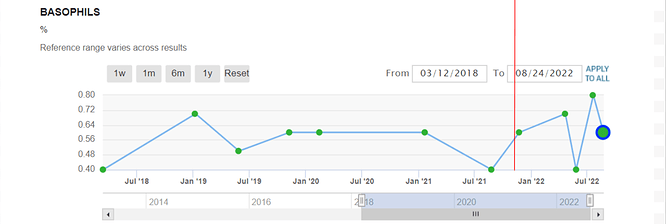
Since Rapamycin is, after all, an immunosuppressant at standard of care dosages for organ transplant patients, we as a community have an opportunity to see if our longevity dosing regimen does or doesn’t have a deleterious effect on our immune system related blood markers.
I would encourage all of you to get a CBC panel (easy to order in US from Life Extension) and report if neutrophils, lymphocytes, monocytes, eosinophils & basophils are in range and report here.
Neutrophil automated: 61.7%
Neutrophil absolute: 3.04 x 103 ul
Lymphocyte absolute: 1.14 x103ul
Lymphocyte Automated: 23.2%
Monocyte absolute: 0.48x103ul
Monocyte Automated: 9.8%
Eosinophil automated: 4.7%
Basophil absolute: 0.02x 103 ul
Basophil automated: 0.4%
All these markers are within normal range all the time.
I’ve been on Rapamune for 12 years, last 6 years I take Rapamune with breaks (7-10 days after the last dose).
The only abnormal marker on my last CBC was Mean Platelet Volume (MPV): 11.3 ( has to be from 7.4 to 11). It’s a little higher than norm. Doc said nothing to worry about. Past results were: 10.6, 10.9, 10.7, 10.3.
Thank you! Great numbers and good to know rapa for 12 years has had no major negative effects.
I am not sure what this tells me as these measurements seem to be all over the place versus time.
The red line is the point at which I started taking rapamycin.
The highest readings seem not to be any higher than the max readings before I started taking rapamycin.
How many previous data points do you have to compare to your current results?
I have been doing weekly blood tests and at times have sent a sample to two separate labs which was taken at the same time. The reason for sending the same sample to two labs is to get an idea as to how precise the results are.
On 16 Jun 2022 I had a white cell count of 2.57 from one lab and 2.75 from another. OTOH a different pair of labs on 23 June gave 3.4 and 3.41. I have a low white cell count not caused by Rapamycin. Looking at Lymphocytes absolute going back I have 0.9, 0.7, 0.8, 0.8, 0.86, 0.87, 0.85. 0.84, 0.85, 0.77, 0.87, 0.76, 0.82, 0.80, 0.90, 0.81, 0.86, 0.78 0.79, and 0.81 from 2022 and 0.9 from May 2021. The last value is post 2mg Rapamycin and I had another test today where I drove the sample to the Lab to get the most reliable results which I hope to receive later today or early tomorrow.
From my point of view it does not appear that 2mg Rapamycin has harmed my white blood cell count, but it is still in a sense early days.
I have posted the before and after blood results in another thread.
My view on Rapamycin is that it should assist in improving mitochondrial quality which should (further) assist in histone acetylation. There is not AFAIK an easy test for this.
I’ve gone back several years (to before rapa) and my counts were not out of range (although did vary like yours) until my most recent test when Lymphocytes were low.
Got another CBC with differential test today, all markers are within normal range again.
Great to hear! Thank you.
I’ve been on rapamycin for about 3 years now (most of the time between 6mg/week to 12mg/week), never had any negative deviations in blood measures of neutrophils, lymphocytes, monocytes, eosinophils & basophils.
Dudley Lamming, researcher at U. Wisconsin, has suggested that ideally we’d like to track and measure “TREGS” (t-cell regulatory cells) to track our immune system health - especially as you go higher in dosing. I’ve yet to find this test at any convenient provider, not managed to get a cost on it. Perhaps someone has some experience with it?
TREGs (T-cell Regulatory Test) (Test details ), Labcorp TREGs test
Test TREGS on the same day you test Trough Sirolimus levels to see if there is significant disruption to your immune system.
More data supporting weekly dosing (not daily) and also taking periodic breaks if you want to improve your immune response. From Peter Attia #118/ Lloyd K. Interferon is a substance in the blood that upregulates a number of amino acids most of which are involved with preventing viral infections. And you need protein synthesis to make all of these proteins. So the worry is that if you inhibit MTOR for a long time, then even though we can upregulate the interferon anti-virual genes, they will not be expressed adequately. You need mTOR to express the proteins induced by interferon.
Rummaging around a bit I think this is all the issue of inhibiting mTor.
See 7.2 in this:
Blocking mTor blocks the proliferation of immune cells in response to IL-2.
Hence I think I am right to keep an eye on the White Blood Cell count.
Blocking mTor, however, enables autophagy and mitophagy to be increased. Given the relatively long half life of Rapamycin I am coming more to the conclusion that it is a mistake to dose too frequently. My initial thoughts are every 4 weeks, but in fact that may be too long a period as the benefits of improved metabolism would occur over quite a long period. It strikes me that a period targeted on autophagy which includes Rapamycin and some fasting and possibly Ferulic Acid need not necessarily be that frequent.
It also seems that it may reduce transcription of HIF 1 alpha which is often quite useful. That is another argument for cycling.
Clearly if you are using it to prevent rejection of a transplant you need to keep it going, but for other purposes there are clearly disadvantages of taking it too frequently.
half life is a little less than 3 days (64h iirc) in 2 weeks around 1/38th is left
True, so after 2 weeks about 1/38th is left, after 64 hours 1/2 is left and 64-128 hours has over 1/4.
Hence if you set the threshold as 1/38th for not inhibiting mTor then it is the time after 2 weeks that is good. However, we don’t know exactly what happens in terms of serum levels or bioavailability inside the cell in all circumstances and it seems clear that mTor inhibition should be cycled. How frequently and with what other exogenous influences (fasting etc) is another question.
The lead author of the 2014 paper suggested That that the vaccines probably would have been just as effective if taken without cycling off of a low dosage of rapamycin, but not effective at a higher dose (20 mg vs 5 mg).
I’ve been taking 3mg of Rapamycin for about 5 weeks.
My eosinophil (absolute) is high. I don’t think it’s related to Rapamycin because it was high on my annual physical in December 2022 (I started Rapamycin in February). I thought I was fighting a sinus infection at the time so I didn’t think much of it.
I just did a CBC & CRP test with Life Extension and it’s still high. I feel fine and don’t have any obvious symptoms.
I’m going to talk to my doctor about it so I’m not soliciting medical advice, but I’m trying to figure it out.
I should also mention that I’m an otherwise healthy 50 year old man.
January 2021 = 315 (normal) - (Quest Diagnostics)
Reference Range: 15-500 cells/uL
Dec 2022 = 614 (Quest Diagnostics)
Reference Range: 15-500 cells/uL
March 2023 = 0.6 (Life Extension)
Eos (Absolute) 0.6 High x10E3/uL 0.0-0.4 HD
Are you taking 3 MG once per week or 3 MG daily?
Sorry, I should have specified. 3mg one time per week. I’m anticipating moving up to 5 or 6mg (once per week), after a bit once I’m confident I’m tolerating it well.
Did you ever get a response or find and answer to this?
No - but to be honest, I have not looked that hard. It would be nice to get this as an inexpensive test available to all. Perhaps we should ask LifeExtensionFoundation or one one of the other groups, to offer this test at a reasonable price for rapamycin users…
Hi all, does anyone know anyone at these groups?