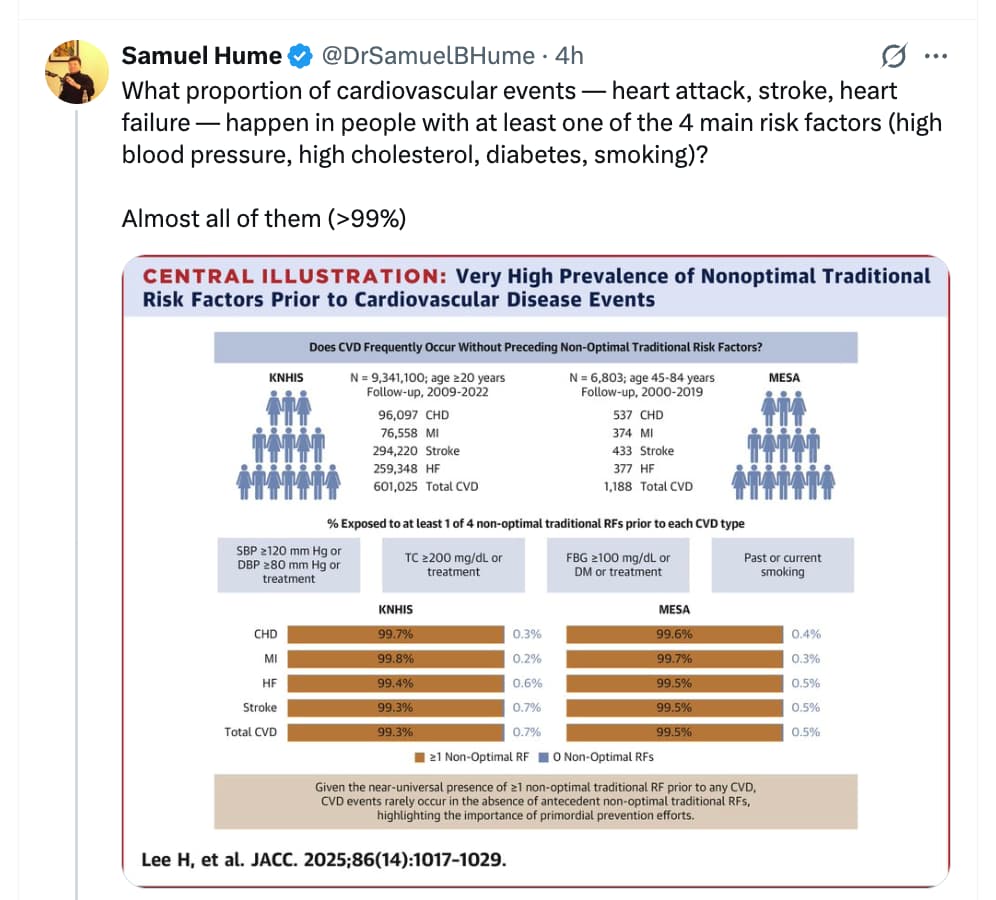
Its interesting… I can see your point. But I take a more risk adverse approach (to my thinking - since CVD is the number one killer of men in North America).
I’ve suffered from higher cholesterol levels much of my life and have taken statins off and on. Now I’m thinking that I want to make sure that cardiovascular health is not my limiting factor as far as healthspan and lifespan go, so I’m being more aggressive and want to get rid of any plaque I have to lower my future risk. So I’ve lowered LDL-C and APO-B to around 45, with statin, bempadoic acid and ezetimibe.
Here is the data on what percent of people have plaque (from Google Gemini 3 Pro):
Estimating the prevalence of cardiovascular plaque—specifically subclinical atherosclerosis—requires distinguishing between clinically diagnosed Coronary Artery Disease (CAD) and the presence of subclinical plaque (detected via imaging like CAC or CCTA). In asymptomatic populations, the prevalence of plaque is significantly higher than clinical diagnosis rates, showing a steep age-dependent gradient.
1. Subclinical Atherosclerosis Prevalence (Aged 40–64)
In middle-aged populations, imaging studies reveal that a majority of asymptomatic individuals already harbor plaque in at least one vascular territory.
- Multivascular Prevalence (Aged 40–54): The PESA Study found that 63% of asymptomatic individuals (mean age 45) had subclinical atherosclerosis in at least one area (carotid, coronary, or ilio-femoral) (Fernández-Friera et al., 2015).
- Coronary-Specific Prevalence (Aged 50–64): The SCAPIS Study utilized Coronary Computed Tomography Angiography (CCTA) and found that 42.1% of the general population had some form of coronary atherosclerosis (Bergström et al., 2021).
| Age Group | Men (Any Coronary Plaque) | Women (Any Coronary Plaque) |
|---|---|---|
| 50–54 | 41.2% | 18.8% |
| 55–59 | 56.6% | 29.3% |
| 60–64 | 68.7% | 40.1% |
| (Source: Bergström et al., 2021) |
2. Coronary Artery Calcium (CAC) in Older Populations (Aged 75+)
In the elderly, the absence of plaque is the exception rather than the rule. Data from the MESA and ARIC studies indicate that coronary calcification (a proxy for advanced plaque) is nearly universal by the tenth decade of life (Miedema et al., 2022).
- Age 75–85: Approximately 89% of individuals have a CAC score > 0, meaning detectable calcified plaque is present. Only 11% of this population has a “zero CAC” score (Miedema et al., 2022).
- Age 90+: Detectable CAC is identified in approximately 95% of individuals across all sex and race subgroups (Miedema et al., 2022).
- High-Risk Burden: Roughly 62.5% of adults aged 75–85 have a CAC score > 100 Agatston Units, which is the threshold typically used to indicate high atherosclerotic cardiovascular disease (ASCVD) risk (Miedema et al., 2022).
3. Clinical vs. Subclinical Disparity
There is a massive gap between the presence of plaque and the manifestation of symptoms.
- Young Adults (18–44): Only about 1% report a clinical diagnosis of CAD, yet early autopsy studies (e.g., the PDAY study) have shown fatty streaks and early plaques in the aortas of most teenagers and the coronary arteries of many individuals in their 20s (ResearchProtocols, 2025; StatPearls, 2024).
- Adults 75+: While ~90% have detectable plaque, only 24.2% report clinical CAD, highlighting a high burden of “silent” atherosclerosis that remains undiagnosed until a major event occurs (ResearchProtocols, 2025).
References
Bergström, G., Persson, M., Adiels, M., Björnson, E., Bonander, C., Ahlström, H., Alfredsson, J., Angerås, O., Berglund, G., Blomberg, A., Brandberg, J., Carlsson, A. C., Cederlund, K., Chen, Y., Coniat, M., Dekkers, R., Duvernoy, O., Ekblom, Ö., Engström, G., … Jernberg, T. (2021). Prevalence of subclinical coronary artery atherosclerosis in the general population. Circulation, 144(12), 916–929. https://doi.org/10.1161/CIRCULATIONAHA.121.055340
Fernández-Friera, L., Peñalvo, J. L., Fernández-Ortiz, A., Ibañez, B., López-Melgar, B., Laclaustra, M., Oliva, B., Mendiguren, J. M., Baguet, J. P., Sánchez-González, J., García, L., García-Huerta, J. J., de Vega, V. M., Zamorano, J. L., Sanz, J., & Fuster, V. (2015). Prevalence, vascular distribution, and multiterritorial extent of subclinical atherosclerosis in a middle-aged cohort: The PESA (Progression of Early Subclinical Atherosclerosis) Study. Circulation, 131(24), 2104–2113. https://doi.org/10.1161/CIRCULATIONAHA.114.014310
Miedema, M. D., Dardari, Z. A., Nasir, K., Blankstein, R., Knickelbine, T., Yeboah, J., Budoff, M. J., McEvoy, J. W., & Blaha, M. J. (2022). Defining demographic-specific coronary artery calcium percentiles in the population aged ≥75: The ARIC Study and MESA. Circulation: Cardiovascular Imaging, 15(10). https://doi.org/10.1161/CIRCIMAGING.122.015145
ResearchProtocols. (2025). Coronary artery disease prevalence in an executive population at a tertiary medical center: Protocol for a retrospective cohort study. JMIR Research Protocols, 14, e72451. JMIR Research Protocols - Coronary Artery Disease Prevalence in an Executive Population at a Tertiary Medical Center: Protocol for a Retrospective Cohort Study
StatPearls. (2024). Risk factors for coronary artery disease. StatPearls Publishing. Risk Factors for Coronary Artery Disease - StatPearls - NCBI Bookshelf